Exploring patients’ experiences of eye injections for neovascular AMD
30 July 2019
Did you know that AMD currently affects about 700,000 individuals in the UK? Statistical models have estimated that these numbers will rise to 3.8 million by 2050. But what exactly is AMD? Here, Christina Yiallouridou from the School of Optometry and Vision Sciences, shares her research into this condition.
Age-related macular degeneration (AMD) is a progressive condition that affects the macula of the eye, and is the primary cause of vision loss in the elderly.
AMD comes in different forms, but advanced neovascular AMD is the only form that can currently be treated with intravitreal (eye) injections. To slow disease progression and maintain good vision however, repeated injections are usually necessary. Lucentis and Eylea are licensed agents in the UK that are used to reduce neovascularisation, clear the excess blood and improve eyesight.
The big BUT
The injections are evident to be safe and effective, but a proportion of patients report experiencing pain and discomfort during or after the treatment. This in turn can cause anxiety and negatively influence patients’ wellbeing and quality of life. It is worth noting that it is a small number of patients who experience pain or discomfort, hence the reason this study focuses on the individual experience.
My PhD
Pain is multidimensional, influenced by clinical procedures, as well as psychosocial factors (sensory, emotional and cognitive aspects). These components add more complexity to the interpretation of the overall experience.
In my research, I will be using subjective, qualitative and physiological measures to investigate the factors associated with both pain intensity and pain quality. In mixed methods research, the integration of qualitative (QUAL) and quantitative (QUAN) approaches can help us understand more about the ocular pain than either measure alone.
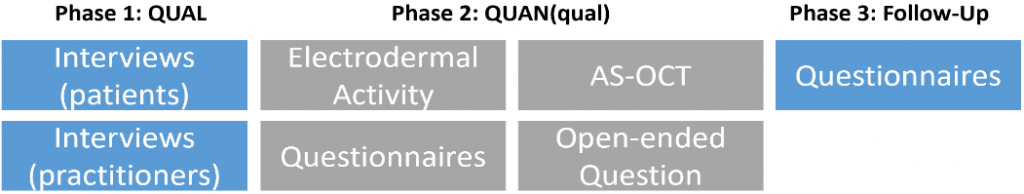
What is known so far?
Pain can depend on procedure-related factors, for example, the effectiveness of the anaesthetic, procedural steps (povidone-iodine application and rinsing, drape placement or removal, placement of the eyelid speculum), the size of the needle and the injection site. Other factors, such as number of injections and regular visits to the hospital, treatment cost, waiting time, pain sensitivity, and pre-treatment anxiety can have an impact on the patient experience, as can aspects that may interfere with the daily routine of the individual such as immobility or lack of transport.
Current Work
The first phase of my study involves interviewing healthcare practitioners to explore their perspectives on the patient experience. Their responses were thematically analysed and summarised below with significant statements and phrases.
Procedure-related factors
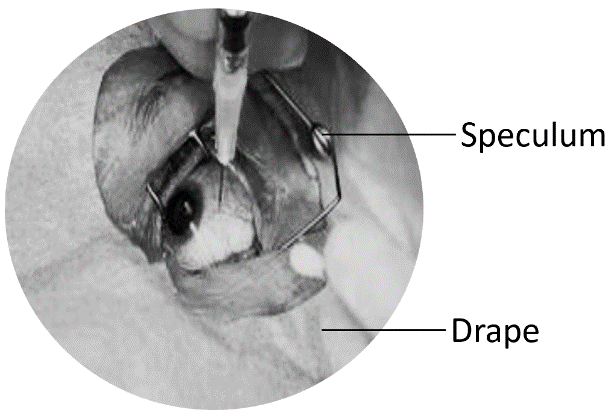
Iodine acts as an antiseptic to protect the eye from infection but it can cause the eye to dry out and lead to discomfort. Patients may also experience claustrophobia when having the drape placed on top of and covering their face. The speculum is an instrument used to keep the eyelids away from the eye during the injection. Patients with smaller eyes may experience higher levels of discomfort or pain because the speculum causes more pressure to the eye.

Psychological factors
Emotional states can affect the pain experience. Negative emotions increase pain, whereas positive emotions have the opposite effect. The thought of having the injection and the preparatory, aseptic procedures used during the treatment are believed to be worse, in terms of anxiety-building, than the actual injection. This may also explain differences in perception between individuals, and differences in pain threshold and sensitivity.

Strategies to improve patient anxiety
Distraction techniques teach patients to shift their attention to stimuli other than the pain, e.g. by imagining a relaxing place, the sounds of waves, etc. Listening to music has been reported to reduce patient anxiety, while relaxation therapy or meditation are similarly effective interventions. Practitioner-patient communication and rapport-building are important considerations when managing patient anxiety. Reassurance is commonly used in clinical practice to remove fears and concerns that patients may have about their illness and treatment. Other strategies adapted to reduce pre-treatment anxiety include hand-holding or hand massage, focusing on the breathing and toes wiggling.

Summary
Patients’ and practitioners’ perceptions differ in many ways. Therefore it is important to study both groups to be able to compare and contrast the two data sets, and identify controversies (if any). Interviewing patients will provide an in-depth understanding of their personal experiences, allowing them to express their opinions, thoughts and feelings about certain aspects of the treatment.
Future work will incorporate pain, anxiety and wellbeing questionnaires, OCT scans of the injection site, and electrodermal activity measurement during the entire injection procedure, with the latter providing a continuous measurement of changing state of arousal and to identify significant painful stimuli.
Christina’s research is funded by The Abbeyfield Research Foundation.
Get in touch with Christina @CYiallouridou
- June 2024
- March 2024
- February 2024
- November 2023
- September 2023
- June 2023
- May 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- July 2022
- May 2022
- April 2022
- January 2022
- December 2021
- November 2021
- August 2021
- July 2021
- June 2021
- February 2021
- January 2021
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- Biosciences
- Careers
- Conferences
- Development
- Doctoral Academy Champions
- Doctoral Academy team
- Events
- Facilities
- Funding
- Humanities
- Internships
- Introduction
- Mental Health
- PGR Journeys
- Politics
- Public Engagement
- Research
- Sciences
- Social Sciences
- Staff
- STEM
- Success Stories
- Top tips
- Training
- Uncategorized
- Wellbeing
- Working from home