Mercy Ships, the NHS, and healthcare systems across the globe – For Alumni, By Alumni
16 July 2020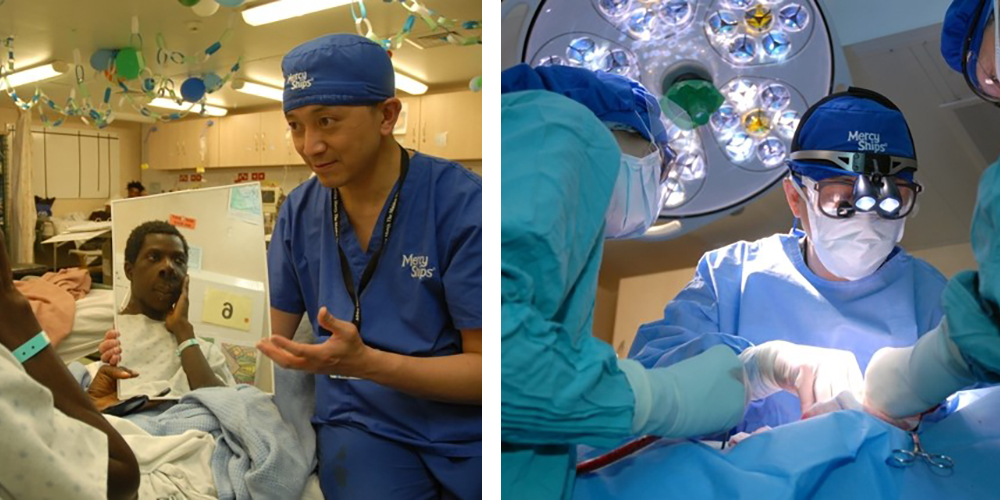
Leo Cheng (LLM 2006) is an oral, maxillofacial, head and neck surgeon who has spent most of his life travelling the globe and helping those from the poorest areas by performing free surgery and providing much needed medical care. He has now turned his attention and efforts to COVID-19 and reflects on his experience so far with the NHS and his concerns for those without a national health system.
For nearly 20 years I have used my annual leave to serve with the Mercy Ships in West Africa, providing free specialist Maxillofacial, Thyroid and Reconstructive surgery to the forgotten poor. Some of my outreach trips have been accompanied by my wife and our two daughters, serving desperate patients together as a couple or a family.
Mercy Ships operates the largest charity-run hospital ship in the world, delivering free, vital medical and surgical care to some of the world’s least developed countries. This floating hospital is staffed by volunteers, who give their expertise for free to help patients with dental and eye problems, facial deformities like cleft lip and palate, tumours of the head, face, neck, limbs and body, club feet, child-birth injuries, burns and many other deformities and conditions.
I was serving the people of Senegal on board the Africa Mercy with my wife Hilary, a Minister from the Methodist Forest Circuit in North East London, when COVID19 started to spread round the world. The situation made it impossible for Mercy Ships to continue our field service as the Africa Mercy is a specialist surgical unit and not equipped to deal with a highly contagious respiratory infection. Within a few weeks of arriving back in the UK, I found myself working overtime in the race against the surge of coronavirus in several London Hospitals.

Apart from urgent cancer and trauma surgery for facial and head injury, my team and I are also providing surgical airway support for those seriously ill COVID-19 patients by making holes in their windpipes (tracheostomy) in order to facilitate their lung ventilation in COVID-19 hospitals.
Operating with Personal Protective Equipment (PPE) has been a learning process as we have to ensure adequate hydration while minimising toilet breaks (tricky at times!), clear articulations to avoid miscommunication with a muffled voice under the FFP3 (N99) mask and visor, alteration of surgical procedures to reduce unnecessary generation of aerosol, extra procedures and checks to reduce the risk of ‘return to operating theatre’, and extended personal hygiene against the invisible enemy.
Although coronavirus has caused extraordinary disruption in all levels of society, it has sped up the embracing of technology and the internet, especially in healthcare. Telephone and virtual clinics have become the ‘new norm’ and teleconferencing has become a major part of my clinical time – connecting with our clinical and management teams, and multidisciplinary cancer team meetings.
During this pandemic, the NHS is looking after everyone in the safest way it can and has generated the capacity to deal with this unprecedented health emergency. Despite the regretful mortality reported daily in the news, there are success stories where COVID-19 patients have left the intensive care unit and walked out of the hospital. Everyone in our nation claps for the NHS and other key workers every week, but the NHS staff also clap for the recovered patients who leave hospital. For instance, a grandmother of three recently beat coronavirus in time for her 74th birthday.
I am extremely grateful and thankful for the resources and provision of our nation’s free world-class NHS, the availability of all basic essential utilities (e.g. electricity, water, gas), food and consumables on supermarkets’ shelves, and sensible expert advice from public health professionals to combat the spread of this invisible enemy.
My experience across the globe means that I know just how fortunate we are and how difficult this pandemic will be for others, especially those in parts of Africa.
Africa is bracing for COVID-19. I heard someone say this: when the global north catches a cold, Africa gets pneumonia. This is because of its poor health care infrastructure and high levels of poverty and lack of education. You can see the unbelievable and huge inequality of health care resources and capabilities between the developed and developing world.
Once the global situation allows, we will return to Africa and help strengthen healthcare systems emerging from the pandemic. The Africa Mercy was there for Guinea in 2016 after Ebola swept across West Africa and we will be there for West Africa after COVID-19.
In this challenging time of lock down and uncertainties with the economy, employment and travel, I hope and pray that we as citizens of this world will come out of COVID-19 more loving and caring towards each other by being generous in helping others within and outside our own community.
Tell us what matters to you
We’ve introduced ‘For Alumni, By Alumni’, because who knows our alumni community better than…you guessed it, you! We’d love to hear from you with ideas for articles or online events that you’re interested in, you can give insight on, or maybe you ARE the story! Check out our full line-up of articles and watch back our live events playlist.
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- November 2016
- October 2016
- September 2016
- July 2016
- June 2016
- May 2016
- April 2016
- March 2016
- February 2016
- January 2016
- December 2015
- November 2015
- October 2015
- September 2015
- August 2015
- January 2015
- December 2014
- November 2014
- September 2014
- August 2014
- May 2014