Idiopathic Pulmonary Fibrosis: my journey to finding a a new treatment
9 April 2019In the first of our blog series on rare diseases, Kasope Wolffs, School of Biosciences, tells us how her research into idiopathic pulmonary fibrosis could change the lives of millions of sufferers worldwide.

Did you know that fibrosis is responsible for almost half of all deaths? If you’re thinking “that can’t be right”, you’re not alone. Sadly, this is the case, since fibrosis is involved in many long-term diseases such as diabetes, asthma and cancer. In addition to playing a key role in the clinical outcomes of these diseases, fibrosis is responsible for diseases affecting major organs, such as cirrhosis of the liver, interstitial lung disease, strabmisus, and keloid scars, as well as cardiac, pancreatic and renal fibrosis. Furthermore, surgery, chemotherapy, radiotherapy and burns can also result in fibrosis.
So what exactly is fibrosis?
Fibrosis is the build-up of scar tissue in response to injury. Upon injury, it is essential for our organs to have the ability to regenerate new cells (replacing damaged ones) and repair the site with no evidence that the injury ever occurred. An obvious example would be our skin, i.e. the formation of a scab after a cut which is replaced by skin cells that look identical to damaged ones, or scar tissue that essentially ensures we’re not walking around with a gaping hole in our arm forever. Like our skin, every organ in our body faces daily assaults which require this wound-healing to occur. In healthy people, native cells ensure our organs function optimally. When these cells are injured by alcohol, smoke particles, pollutants, etc., the wound-healing process is activated to resolve the injury and restore function. However, in fibrosis, scar-forming cells hijack this process releasing signals that attack native cells and take over. These scarred organs can eventually fail and in most cases lead to death.
When you type ‘fibrosis’ into Google, most of the results on the first page focus on pulmonary fibrosis, or lung fibrosis. This might be because our lungs play one of the most important jobs in the body – getting oxygen in and carbon dioxide out. Anything that disrupts this balance results in suboptimal function of the other organs in the body. There are over 200 conditions under the umbrella term pulmonary fibrosis. The most common is idiopathic pulmonary fibrosis (IPF), meaning the cause is unknown. There are an estimated five million people living with IPF worldwide. It is considered a rare disease with a prognosis worse than most cancers. Once diagnosed, survival is 3-5 years for 50% of IPF patients.
The need for new treatments
Currently, the only effective treatment is lung transplantation, which is not a viable therapeutic avenue for most patients due to their advanced age or the presence of co-existing diseases. The two existing FDA-approved drugs don’t improve patient quality of life and are associated with severe side effects. This means there is a drive to develop a breakthrough drug which improves survival, symptoms and quality of life. This is the focus of my PhD.
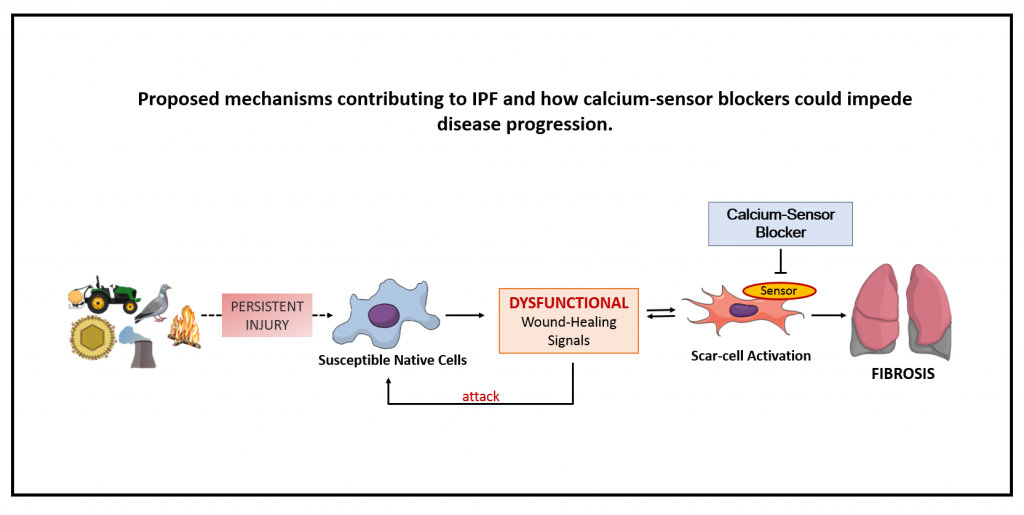
In IPF, fibroblasts (cells which lay down scar tissue in response to an injury) are too active, and gradually replace the small air sacs in the lungs with scar tissue – making them stiff and thick. This eventually hinders the lungs’ ability to transfer oxygen into the body. In this dysfunctional state, fibroblasts release signals, which are picked up by sensors on surrounding cells. One of these sensors is known as the calcium sensor. The calcium sensor has been shown to be hyperactive in diseases such as asthma and hypertension, and blocking the sensor’s activity with drugs can reduce scarring. Results from the first year of my PhD showed that when healthy fibroblasts are made to act like IPF fibroblasts, treatment with calcium-sensor blockers reduced scarring. This suggests that these drugs might be effective in the treatment of IPF. I am currently working on showing that the sensor blockers can prevent scarring in diseased fibroblasts (from IPF patients).
Although we are a long way from the clinic, my PhD aims to develop a drug that might make a difference to millions of IPF patients worldwide.
Comments
2 comments
Comments are closed.
- March 2024
- February 2024
- November 2023
- September 2023
- June 2023
- May 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- July 2022
- May 2022
- April 2022
- January 2022
- December 2021
- November 2021
- August 2021
- July 2021
- June 2021
- February 2021
- January 2021
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- Biosciences
- Careers
- Conferences
- Development
- Doctoral Academy Champions
- Doctoral Academy team
- Events
- Facilities
- Funding
- Humanities
- Internships
- Introduction
- Mental Health
- PGR Journeys
- Politics
- Public Engagement
- Research
- Sciences
- Social Sciences
- Staff
- STEM
- Success Stories
- Top tips
- Training
- Uncategorized
- Wellbeing
- Working from home
My mum was diagnosed with pulmonary fibrosis yesterday. Thank you for your research.
Wishing your mum all the best, Becky. Hoping the research in this field keeps going forward!