Investigating the link between ADHD and depression
4 February 2019Victoria Powell, PhD Researcher, School of Medicine (Division of Psychological Medicine and Clinical Neuroscience)

During this year’s Children’s Mental Health Week, undoubtedly there will be children and adolescents with Attention-Deficit Hyperactivity Disorder (ADHD) receiving mental health support up and down the UK. ADHD is one of the most common neurodevelopmental disorders and it is associated with a range of mental health problems later in life including depression.
A child with ADHD will typically have difficulty focusing on tasks and may at times feel so full of energy that they struggle to even sit still. This kind of hyperactivity may seem worlds apart from depression – a mental health condition characterised by low mood and energy amongst other symptoms. However, studies are increasingly showing a link between ADHD in childhood and depression in later life.
In fact, one study by Fergusson et al. in 2010 showed that of those with ADHD in adolescence, 50% had depression by early adulthood. However, while research shows that ADHD seems to be linked with depression later on, the reasons behind this link are still unclear. Investigating the risks that link ADHD and depression is essential in identifying how we might be able to treat or prevent depression in those with ADHD.
The focus of my PhD so far has been investigating the role of academic and friendship difficulties in the ADHD-depression link. Children often find that their ADHD makes it difficult to make and maintain good friendships, in addition to hindering progress at school. Both of these difficulties can also lead to depression. Therefore, I wanted to investigate whether there is a pathway by which some children with ADHD experience increased friendship and academic difficulties which in turn damages their self esteem and elevates depression risk.
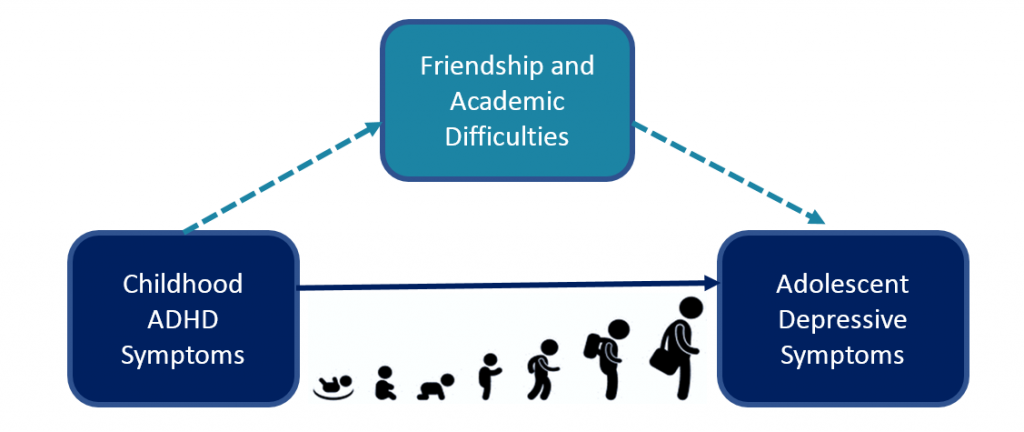
My findings in a study of over 2000 individuals from the Avon Longitudinal Study of Parents and Children (ALSPAC) support this theory. Results showed that childhood ADHD symptoms are associated with adolescent depressive symptoms 10 years later, with friendship and academic attainment difficulties explaining around 15% and 20% of this ADHD-depression link, respectively. This remained the case even when we accounted for the potential effects of socioeconomic background, gender, childhood emotional problems and IQ on our results. This highlights friendship and academic difficulties as important potential targets of depression prevention and intervention programs in those with ADHD.
While drawing attention to the role of friendships and academic achievement is important however, this is far from the full picture of the ADHD-depression link. There will be many more routes and reasons behind the association of ADHD and depression, both environmental and genetic. Research is beginning to uncover these routes, hopefully with new clinical implications for depression prevention and treatment for children with ADHD on the horizon.
Get in touch with Victoria @VictoriaIPowell
Comments
2 comments
Comments are closed.
- March 2024
- February 2024
- November 2023
- September 2023
- June 2023
- May 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- July 2022
- May 2022
- April 2022
- January 2022
- December 2021
- November 2021
- August 2021
- July 2021
- June 2021
- February 2021
- January 2021
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- Biosciences
- Careers
- Conferences
- Development
- Doctoral Academy Champions
- Doctoral Academy team
- Events
- Facilities
- Funding
- Humanities
- Internships
- Introduction
- Mental Health
- PGR Journeys
- Politics
- Public Engagement
- Research
- Sciences
- Social Sciences
- Staff
- STEM
- Success Stories
- Top tips
- Training
- Uncategorized
- Wellbeing
- Working from home
Hey, thank you very much for the information! Is there a way I can get more info on the matter? So I can make a post on my local university about this? Thank you very much in advance!
Hi. Thanks for your message. You can get in touch with the author of this piece – Victoria Powell – at @VictoriaIPowell on Twitter. Hope this helps!